Is that tricky American English R getting you down?
Maybe you’ve been waiting and hoping your school-aged child would eventually stop turning R into W on her own. Maybe your son is finishing his third year of school-based speech services, has made good overall progress, but still cannot quite get that R sound to click.
Whatever your story, you are not alone. Difficulty with the American English R is extremely common. In fact, the R sound we use in American English is a relatively rare version of R compared with many other languages.
I like to think that has something to do with how complex the sound is from a phonetic standpoint. That may not be the actual reason, but after nearly twenty years of helping children work through this exact sound, I can say this with confidence: if your child is struggling with R, it makes sense.
The good news is that there are practical steps you can take to help.
Why the R Sound Is So Difficult
Let’s start with a quick crash course in phonetics.
R is difficult because it is one of the main consonant sounds in English that requires very precise, coordinated movement. In other words, your child has to do several things at the same time for the sound to come out correctly.
For a clear American English R, three things need to happen:
- The lips need to round. This is one reason an incorrect R can sound so much like W.
- The tongue needs to create a hump in the mouth, either by rolling slightly backward or retracting.
- The root of the tongue needs to pull back, similar to what happens when you gargle.
All of that has to come together at once. So if your child is still finding R difficult, that is completely understandable.
Now let’s talk about what you can do to help.
Start With the Tongue, Not the Lips
I’m going to move quickly past the first piece: lip rounding.
In my experience helping kids with R, lip rounding is almost never the core problem. It may be part of the sound, but it is rarely the main reason a child cannot produce R correctly.
The real issue is usually the second piece: creating that hump with the tongue.
This is often the missing link. A child may understand what the sound should be. They may have heard instructions from a therapist, seen drawings, and practiced again and again. But they still may not know exactly where the tongue should go or what it should feel like.
That is one of the reasons we developed Speech Buddies Tools. The goal was to provide a direct cue that helps children feel and understand what the tongue needs to do, rather than relying only on verbal instructions.
For many kids, that tactile cue creates an “Aha!” moment. All of those explanations and diagrams get distilled into one clear action.
With the Speech Buddies R Tool, the tongue tip moves to the small bumps that show the starting position of the tongue. Then the child simply unrolls the coil.
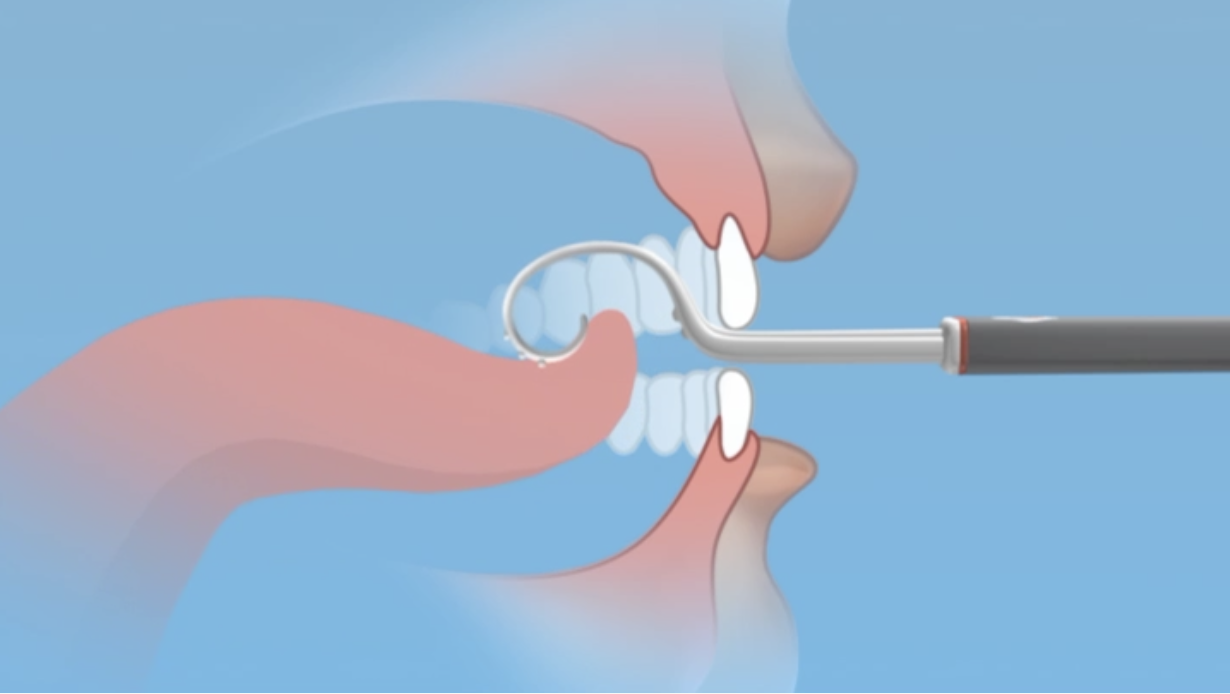
That’s it.
Of course, it can take time for a child to get comfortable with the setup, and consistent practice still matters. But for thousands of children, this kind of direct cue has provided the missing piece in their R practice.
If R Still Is Not Clicking, Check the Tongue Root
If your child is using the Speech Buddies R Tool correctly and still is not quite getting the sound, the issue may be the third piece: tongue root retraction.
A practical way to teach this is to have your child practice R while gargling a small amount of water.
Gargling is an exaggeration of what is needed for R, but that is part of why it can be helpful. It gives your child a clear sense of the tongue-root movement involved in the sound.
Once these pieces begin to work together, your child can start getting those first accurate R sounds under his or her belt.
Practice Matters, Especially Early On
As I mentioned earlier, diligent practice is essential.
Early in the process, use the Speech Buddies R Tool for most practice repetitions. Then, as your child’s accuracy improves, gradually fade the tool and see whether your child can produce the sound independently.
Be sure to practice a variety of R sounds, including R at the beginning, middle, and end of words, as well as R in clusters such as br-, cr-, gr-, and str-.
You can also use your preferred AI tool to help generate practice word lists. For example, you might use a prompt like this:
Give me a twenty-word list of one- and two-syllable words containing R. I want R in each word only once, and the list should mix up where R occurs in the word, including the beginning, middle, and end of words, as well as clusters.
Practice the list once a day for several weeks. It can also help to choose a small reward your child can look forward to after putting in the work.
Once your child becomes more accurate with single words, move those words into short five- to eight-word sentences. The sentences do not need to be fancy. Just think of a simple sentence that includes the target word and gives your child another chance to practice R in a more natural context.
Keep Going
R can be stubborn, but it is not impossible.
With the right cues, consistent practice, and a little patience, your child can make real progress. Keep at it, celebrate the small wins, and let us know how it goes.
At Speech Buddies, we’re dedicated to helping kids make meaningful progress toward their speech goals. If you have questions about how our tools can best be used in speech therapy, or need help finding an SLP, contact us today.






