Speech Therapy for Paradoxical Vocal Fold Movement (PVFM)
Communication is so vital for navigating the world around us. These days, pretty much everybody has their own cellphone (or two…) and you can’t walk down the street without bumping into somebody texting or yammering away into their Bluetooth headset. But what if you found yourself suddenly unable to speak? Even worse, what if you could barely breathe? If you had paradoxical vocal fold movement (PVFM), this scenario would be commonplace for you. Fortunately, speech therapy can help.
What Is It?
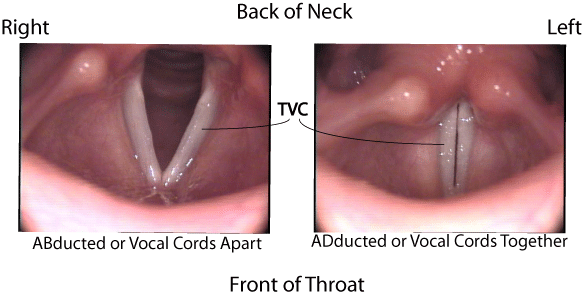
Paradoxical vocal fold movement is also sometimes called vocal cord dysfunction (VCD) or vocal cord malfunction. It is a type of voice disorder. PVFM is also an involuntary function disorder. It involves the glottis, which is defined as a person’s vocal folds, or vocal cords, along with the rima glottidis, which is the space between the vocal folds.
Most of the time, a person with PVFM can breathe and speak normally. Periodically, an episode can occur in which there is a glottic closure that may be greater than 50%. In nonscientific terms, the throat closes up while the patient is trying to inhale.
What Are the Symptoms?
Paradoxical vocal fold movement is often misdiagnosed as asthma because a person with the disorder will exhibit many of the same symptoms during an episode. Wheezing and difficulty breathing will occur. However, PVFM can be differentiated from asthma in that a person with asthma will typically have trouble breathing out, rather than in. If your child is diagnosed with asthma but treatment does not appear to be improving his symptoms, have him evaluated for PVFM instead. Your child might also complain about pain in his throat, and you might notice a change in voice quality or a loud noise upon inhalation during an episode.
Is PVFM Treatable?
Yes, the good news is that with the help of a speech-language pathologist (SLP), your child can overcome PVFM. According to an article originally published in Contemporary Pediatrics, an average of 3.7 speech therapy sessions for 59 children resulted in a 63% success rate. So unlike some speech disorders like severe lisps or apraxia, PVFM may not require years of intensive speech therapy. However, it’s always a good idea to consult the speech therapist about activities to do at home to accelerate your child’s progress. For example, if your child also struggles with an articulation disorder, using Speech Buddies for a few minutes a day can help him.
Psychiatric Treatment for PVFM
Speech therapy techniques can be helpful by themselves, but children who also have an underlying psychiatric disorder require psychiatric treatment. According to that same article in Contemporary Pediatrics, about 75% of children with PVFM may also have an underlying psychiatric disorder that can aggravate symptoms of PVFM. Your child’s SLP might recommend that he be evaluated by a psychiatrist.
Speech Therapy Assessment
In addition, your child’s speech therapist should conduct her own assessment, which is likely to include a structural and functional exam of the speech structures, an assessment of musculoskeletal tension in the laryngeal area, and a measurement of respiratory pressure.
Speech Therapy Techniques for PVFM
The first step in teaching a child how to control his breathing should be to educate him about how breathing occurs. Patient education often goes a long way toward establishing normal vocal fold control, particularly when the SLP does not find any abnormalities of the speech structures. The SLP will tailor the language used in patient education to the child’s age and comprehension.
Then, the SLP will likely work with your child on laryngeal breathing techniques and control exercises. Your child will be guided through muscle tension and releasing exercises to teach control over the laryngeal area. This also helps the youngster learn to identify when tension begins to build up before an episode so that he can release the tension.
Your child will also likely learn the relaxed-throat breathing technique, in which he is guided through a series of breathing exercises. He will first learn this technique in a relaxed setting, and then he will be encouraged to practice it in situations that may trigger his PVFM episodes (i.e. during sports activities). Work with the speech therapist to learn how to guide your child through these exercises at home, as well.